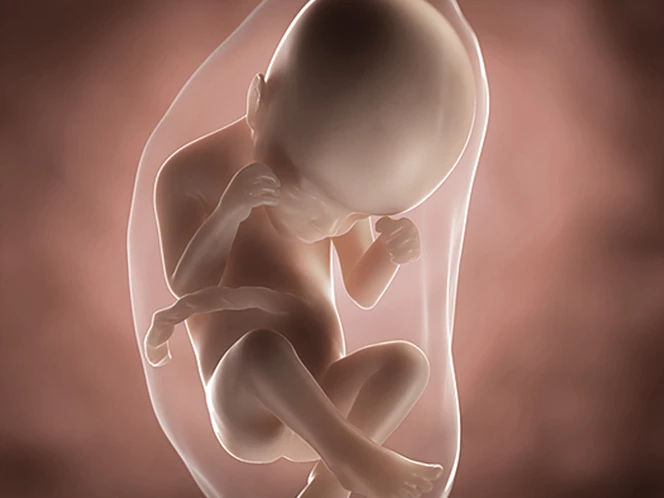
In week 24 of pregnancy, your baby is around 21cm long from the crown of its head to its bottom, roughly the same size as an ear of corn, only heavier. It should weigh around 600g.1,2
Your baby is pretty much complete now, if a little on the skinny side. He or she will continue to plump out over the coming weeks. Your baby also now has all their facial features, including eyebrows and eyelashes – they may even have some wisps of hair growing1.
A substance called ‘surfactant’3 is appearing inside your baby’s lungs. It helps keep the tiny air sacs in his or her lungs (alveoli) open. Your baby has been practicing breathing since around week 17 so, if they were to arrive prematurely, they’d have a good chance of surviving and breathing without the aid of a neonatal unit.